Parkinson’s disease affects nearly one million Americans and millions more worldwide. Researchers are now testing a remarkable new technology sometimes described as a “pacemaker for the brain.” This device can monitor brain activity in real time and automatically adjust electrical stimulation to control symptoms.
A recent report from CNN describes how this technology — known as adaptive deep brain stimulation — may significantly improve symptom control for some people living with Parkinson’s disease. If successful, it could represent a major step forward in how neurological disorders are treated. You can read the original report here: How a “Pacemaker for the Brain” Could Help Treat Parkinson’s.
Below is a closer look at how this technology works and what it may mean for patients and families.
What Is a “Brain Pacemaker”?
Deep brain stimulation (DBS) is not new. Surgeons have been using DBS for more than two decades to treat certain Parkinson’s symptoms such as tremor, rigidity, and slowed movement. According to the National Institute of Neurological Disorders and Stroke, the procedure involves implanting thin electrodes into specific regions deep in the brain.
Those electrodes connect to a small battery-powered device implanted under the skin of the chest. The device sends carefully controlled electrical pulses to regulate abnormal brain activity.
Doctors often compare DBS to a cardiac pacemaker. Just as a heart pacemaker stabilizes abnormal heart rhythms, DBS can help stabilize abnormal brain signals that cause Parkinson’s symptoms.
Traditional DBS, however, delivers constant stimulation, even though the brain’s needs fluctuate throughout the day.
The New Innovation: Adaptive Deep Brain Stimulation
The newest generation of DBS devices adds an important feature: the ability to monitor brain signals and adjust stimulation automatically.
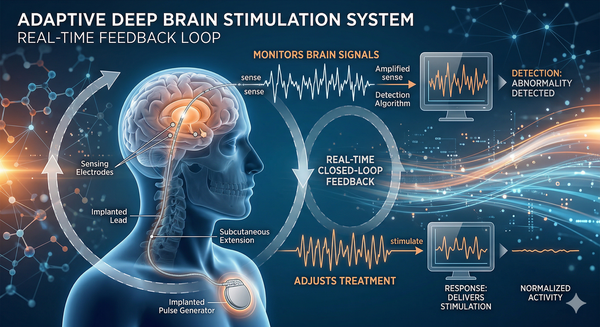
This approach — known as adaptive DBS — functions as a closed-loop system. Instead of providing a fixed level of stimulation, the device continuously analyzes brain activity and responds in real time.
Researchers at the University of California, San Francisco, describe this approach in detail in their research on adaptive deep brain stimulation for Parkinson’s disease. The device detects abnormal brain-wave patterns linked to Parkinson’s symptoms and increases or decreases stimulation accordingly.
This means stimulation is delivered only when needed, which may improve symptom control and reduce side effects.
What Symptoms Can It Improve?
Parkinson’s disease disrupts brain circuits that control movement. As those circuits become less effective, patients may experience:
• Tremors
• Muscle stiffness
• Slowness of movement
• Involuntary movements caused by medication
Adaptive DBS aims to stabilize the abnormal brain activity that produces these symptoms. Early research funded by the National Institutes of Health suggests that adaptive stimulation can reduce symptom fluctuations and improve overall control compared with traditional DBS. Details of that research are summarized by the NIH in its report on self-adjusting brain stimulation devices for Parkinson’s disease.
Some patients in early trials also reported fewer medication side effects and more consistent symptom control throughout the day.
Recent Advances and Regulatory Progress
The technology has moved rapidly from research labs to clinical use. In 2025, the US Food and Drug Administration cleared certain adaptive DBS systems for use in patients with Parkinson’s disease.
The CNN article describes several patients who participated in early trials of the technology and experienced substantial improvement in their mobility and daily functioning.
While the treatment does not cure Parkinson’s disease, it may help many patients manage symptoms more effectively — particularly those whose symptoms fluctuate widely despite medication.
Who Might Be a Candidate?
Deep brain stimulation is generally considered when Parkinson’s medications no longer provide consistent control of symptoms.
Patients may be evaluated for DBS if:
• Tremors or movement problems significantly interfere with daily life.
• Medication side effects become difficult to manage.
• Symptoms fluctuate dramatically throughout the day.
Because the treatment involves brain surgery, careful medical screening is required to determine whether a patient is a good candidate.
The Broader Future of Brain-Based Therapies
Adaptive DBS is part of a growing field called neuromodulation — the use of electrical stimulation to regulate abnormal brain activity.
Researchers are exploring whether similar closed-loop systems could eventually treat other neurological conditions, including epilepsy, depression, obsessive-compulsive disorder, and chronic pain.
While these treatments remain under investigation, they illustrate how rapidly neuroscience is evolving.
Why This Matters for Families
For families living with Parkinson’s disease, maintaining independence and quality of life is often the greatest challenge.
Innovations such as adaptive deep brain stimulation may not cure the disease, but they offer something extremely valuable: better control of symptoms and potentially more years of functional independence.
As research continues, technologies that once sounded like science fiction — such as a “pacemaker for the brain” — are becoming real tools that can improve the lives of people facing serious neurological illness.
Get in Touch or Schedule Your Consultation
Don’t wait for a crisis. Educate yourself, talk with those you trust, and work with a knowledgeable attorney here at the Farr Law Firm to make your decisions official.